How to Use an AED in Tallahassee: Step-by-Step Guide for Emergencies
The first few seconds after a person drops, stops responding, and everyone in the room looks at each other are where AED hesitation actually lives. The device itself is rarely the hard part. The hard part is the pause before anyone in a Midtown restaurant kitchen, a downtown Tallahassee office tower, or a hotel ballroom along Apalachee Parkway commits to taking the cabinet off the wall.
An AED is engineered to take pressure off that moment. Once it powers on, it speaks aloud, reads the heart rhythm, and tells the rescuer whether a shock is advised. The job left for the person holding it is mechanical: get the pads on the patient, follow the prompts in order, and return to CPR after each analysis or shock.
Knowing the sequence matters more than knowing the technical language, because a person who has rehearsed the order is much less likely to freeze when it counts. That matters in any building stocking a public AED across Leon County: the concourses at Tallahassee International Airport, the lobby at the Donald L. Tucker Civic Center, the corridors of an office park off Mahan Drive. The people already nearby become the first responders whether they signed up for the role or not.
Educational note: use this information for general awareness only. It is not a substitute for calling 911, hands-on training, or professional medical judgment during an emergency.
Upcoming CPR Class Dates and Times
Know When the AED Belongs in the Response
The AED belongs in the response the moment a person is unresponsive and is not breathing normally, or is only gasping. That pattern points to sudden cardiac arrest, not a faint, a panic attack, or somebody who needs a minute and a glass of water.
A patient who is awake, talking, or breathing in steady cycles is a different kind of emergency. If the person is on the floor and not responding, the path is immediate: call 911, start CPR, and send a second person to get the AED moving toward the patient.
Most hesitation comes from wanting perfect certainty before doing anything. Cardiac arrest does not give you that kind of time. If the person is unresponsive and is not breathing normally, you move.
Step 1: Turn It On and Follow the Prompts
Turn the AED on the moment it reaches the patient. Most units begin speaking the second they power up, which is the entire point in a high-stress scene with adrenaline running through everyone in the room.
The voice prompts walk through the sequence in order. They tell the rescuer when to attach the pads, when to step back, and when to resume CPR. Nobody is expected to invent the rescue in real time or recite the steps from memory while a person is on the floor.
That built-in coaching is one reason public AEDs work as well as they do for first-time users. The machine handles the analysis and the audio cues. The rescuer handles the physical work: turning the device on, placing the pads correctly, clearing the patient when told, and going right back to compressions when told.
Step 2: Expose the Chest and Place the Pads
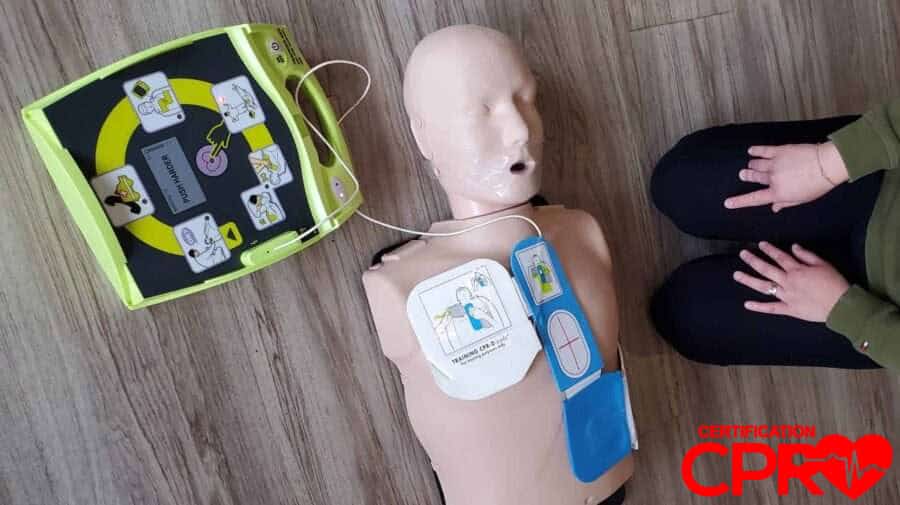
Pads go on bare skin, not over a shirt or bra strap. The diagrams printed on the pads themselves show exactly where they belong, and following those pictures matters because the placement is what allows the device to read the rhythm correctly and, if needed, deliver a shock through the heart.
For a typical adult rescue, one pad goes on the upper right side of the chest and the other goes on the lower left side. That layout creates the path the device expects to use. In a hands-on AHA BLS class in Tallahassee, students practice that placement on a manikin as part of the full CPR-and-AED sequence so it feels familiar instead of theoretical when the real moment arrives.
If the chest is wet, dry it quickly before applying the pads. The pool at Premier Health & Fitness, the swim deck at the FSU Reservation, locker rooms off Tennessee Street, and outdoor events at Cascades Park during a summer concert are all settings where that adjustment comes up. If the patient has a pacemaker or a visible implant under the skin, place the pad slightly off to the side of it instead of directly over it. None of those are reasons to stall out or back away from the rescue.
Step 3: Clear the Person During Analysis and Shock
Once the pads are attached, the AED analyzes the rhythm. Nobody touches the patient during that read. The machine needs a clean signal, and this is one of the moments where scene control matters most.
Look at the patient, look at the people around you, and say "clear" out loud so everyone steps back. If the device advises a shock, stay clear again while the shock is delivered. This is not the moment for quiet assumptions or hoping the bystanders behind you noticed what is happening.
This is the part people rush in a crowded room. Someone keeps a hand on the patient’s shoulder. Someone else leans in to look. A third person keeps repositioning the body while the device is working. One clean, confident clear command from the rescuer keeps the response safer and tighter, and it keeps that pause short so compressions can resume.
Step 4: Resume CPR Right Away
After the AED analyzes the rhythm, it either advises a shock or announces that no shock is advised. The response is still moving in either case, and the next step is almost always to resume CPR the moment the device says so.
If the shock is delivered, resume compressions when the machine prompts. If no shock is advised, resume compressions when the machine prompts. Some bystanders hear "no shock advised" and treat it like a stopping point, as if the emergency has somehow downgraded. It has not. The phrase only means the device did not detect a shockable rhythm at that moment, so compressions need to keep going.
That back-and-forth between CPR and AED prompts is the actual rhythm of the rescue. The device checks. The rescuer pushes. The cycle repeats until Tallahassee Fire Rescue or Leon County EMS takes over, or until the patient starts showing clear signs of life. Once the rescuer understands that pattern, the whole process feels much less mysterious.
Mistakes That Slow AED Use Down
The most common mistake is hesitation at the start. People burn the most valuable seconds wondering whether they are qualified, whether someone else is on the way, or whether using the AED could somehow make things worse. The device is on the wall for exactly this moment, and using it is what it is there for.
The second most common problem is poor scene control. Too many people crowd in, nobody gives a clear command, and somebody is still touching the patient during analysis. A step that should take a single moment turns messy because nobody on the scene has taken charge of it.
Upcoming CPR Class Dates and Times
The third loss of time comes from treating the AED as if it replaces CPR. It does not. CPR and AED use belong together. If compressions stop for too long after each prompt, or if everyone stands around waiting for the device to finish thinking, the response slows down and the rescue loses momentum.
Hands-on practice is the fix here, because the sequence has to live in the rescuer’s hands and not just in their head. The kind of emergency that ends in survival usually begins somewhere ordinary: an office break room near Kleman Plaza, a hotel corridor off North Monroe Street, the Lawton Chiles gym. The AED is already on the wall in those buildings. Whether it gets to the patient quickly is a question of how familiar the sequence felt to the first adult in the room before that day arrived.
